Connection between informed consent and patient participation?

Table of contents

This blog describes the essence of patient participation and shows you that informed consent in an important form of patient participation.
What is patient or client participation?
Patients or clients look at healthcare from a different perspective than healthcare professionals. They have specific expertise that is unique and related to their personal situation, their treatment, their disease and their recovery. In order to take full advantage of this expertise, the organisation and healthcare professional should align buyer and supplier perspectives for the organisation of medical care.
Patient or client participation is a means to use the patient’s/client’s perspective to define patient/client-centred care.
This means that patients and clients have the opportunity to share their knowledge and experience that may contribute to improvements in healthcare. A patient may be an individual patient, but also a group of patients or patients’ representatives, like parents and patients’ relatives.
The ladder of participation
The form of patient and client participation depends on the way they get involved, on the objective of the participation and the project you want patients/clients to participate in. Patients can merely be informed, but they can also be asked to participate in the decision-making process for certain issues. The ladder of participation is used to clarify the difference in levels of participation between the five forms of participation.
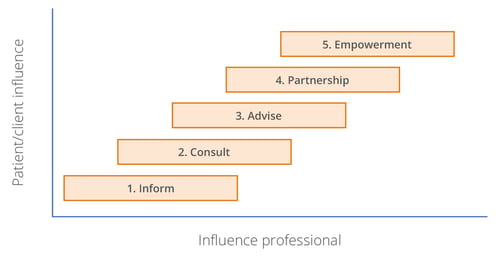
Improve the quality of care
Good quality care means that the care (among other things) is patient/client-centred. Each patient has his own specific preferences, needs and problems. 'The' patient does not exist. It is therefore important to involve patients regularly. “Patient- or client-centred does not mean “Your wish is our command!” but it does mean diversity in service provision. It allows for tailor-made approaches and clarifies the service (im)possibilities to the patient”.
What is informed consent?
Before a doctor performs a medical intervention, the patient or client has to give his consent. This is a key principle of health law. Without this consent there is an unauthorised infringement of the patient’s safety. In order to give consent, however, the patient needs good information. Before asking for consent, a doctor therefore has to first give the patient information about the intended examination or the proposed treatment.
“The doctor’s obligation to provide information and the consent requirement go hand in hand. It is also called informed consent”
From a legal point of view, compliance with informed consent by doctors is important. There is, however, an additional important benefit. Research has shown that informing patients/clients about the medical treatment creates a foundation for mutual trust and promotes therapy compliance.
Incident reporting by patients and clients
During the informed consent conversation, the doctor can at the same time mention and stress the importance of patient and client experiences. Inform patients/clients that they have the opportunity to share their experiences that contribute to improvements in healthcare. Since patients, clients, as well as their relatives, are the only ones who pass through the entire care process, they can best pinpoint the weak links within the care process. When patients get the opportunity to report (near) incidents, weaknesses become clear and safety of care can be improved. It is important though to indicate what happens with the reports. Because incident reporting is an important form of participation, a professional follow-up is equally important. Read more on our incident management solution page.
How can The Patient Safety Company support participation?
TPSC CloudTM software supports the use of patient/client participation. By using a variety of tools, patients and clients can easily provide feedback on the care provided, for example by completing an online satisfaction survey. This feedback can then be discussed in the workplace. Weaknesses within existing processes are highlighted, analysed and optimised.
Any patient or client can report (near) incidents by completing an online form that can be easily filled in and that can be accessed via desktop and mobile devices. The form can be tailored to the individual needs of each health organization. When completing the reporting form, the answers are carried over straight away to an analysis method, so that the safety committee can easily identify the causes of the incident and initiate improvement actions..
Each step of the Incident Management System can be easily carried out. While handling the (near) incidents, the safety committee is supported by automated e-mail notifications, reports and alerts.
eBook about Patient participation
Do you want to know more about patient participation? Download our eBook 'How do you turn regular care into excellent care?':
Related articles
-
 Patient safety Incident management Reporting data Quality management
Patient safety Incident management Reporting data Quality managementThe importance of incident reporting in nursing
Work accidents and incidents happen in every industry, including nursing. This article shows how reporting can help increase patient safety.
Read more -
 Communication TPSC News Organization
Communication TPSC News OrganizationServicedesk Engineer Mitch Dobbe | TPSC
Curious about the work of The Patient Safety Company's servicedesk? Read our interview with Servicedesk Engineer Mitch Dobbe!
Read more -
 Communication TPSC News Organization
Communication TPSC News OrganizationSecurity Officer Pardi Scheffer | TPSC
Curious about the work of The Patient Safety Company's servicedesk? Read our interview with Senior Servicedesk Engineer Pardi Scheffer!
Read more
